Disclaimer: This intensely personal narrative is shared with the profound hope that it encourages, rather than discourages, anyone contemplating birth or natural birth. Every birthing journey is uniquely personal and profoundly different. This account merely chronicles my specific experience with this particular birth. If you find yourself in a space where reading a challenging birth story might be unsettling, you might consider skipping this blog post for now.

Five months have gracefully passed since my little man made his grand entrance, and I’ve finally found the emotional space to commit his birth story to writing. For a long time, I questioned if I would ever share this deeply intense and prolonged experience. The raw memories were overwhelming, but with the gift of time and perspective, I’ve realized that despite its undeniable difficulty, it holds an intrinsic beauty. It’s the powerful testament to how my son fought valiantly to enter the world, and how we both battled fiercely to meet each other. This is not just a birth story; it’s a saga of endurance, love, and the incredible bond forged in the crucible of labor.
A quick note of transparency: certain details within this account will be deliberately vague. The events unfolded over several days, marked by immense stress and minimal sleep, making some memories hazy. What I recount here is my truth, as vividly as I can recall it, hoping to offer an authentic glimpse into our journey.
Navigating Pregnancy and Birth Amidst the 2020 Lockdown
The spring of 2020 will forever be etched in collective memory, a period defined by nationwide lockdowns and unprecedented uncertainty. While everyone’s relationship with these events varied, we can never diminish the frightening and emotionally taxing reality faced by pregnant mothers and new parents during that time. The world felt like it had turned on its head, and the prospect of bringing a new life into such a volatile environment was profoundly unsettling.
I am incredibly grateful that my entire pregnancy journey was marked by good health, a blessing I often reflected upon (you can read more about my first and second-trimester recap). Everything was meticulously planned for a natural, unmedicated delivery at our chosen birthing center, right around my April 16th due date. Then, March 13th arrived, and with it, a seismic shift in our comfortable, familiar world. Fears for our health escalated, reports surfaced of mothers separated from their newborns, and partners being barred from labor rooms. My previously joyful and personal midwife visits transformed into impersonal televisits, punctuated only by brief, essential vital checks. Our carefully crafted birth and postpartum plan, which included welcoming family for support, crumbled instantly.
In those final weeks of pregnancy, we were physically isolated, confined to our home. I vividly recall sitting in the nursery’s rocking chair, tears streaming down my face, overwhelmed by the sheer uncertainty of everything. I grieved the loss of a “normal” birthing experience, a comforting rite of passage denied by global circumstances. Most acutely, I feared for my unborn son’s well-being in this new, bewildering world.
The emotional toll was immense. I became incredibly edgy, rarely venturing out or seeing anyone beyond my husband, Daniel, and our midwives. While I can never definitively pinpoint the exact cause for the arduous path my labor took, I strongly believe that my mental state during the lockdown – a constant undercurrent of anxiety and fear – did not serve me well as I approached the threshold of motherhood.
The Deceptive Dawn of Prodromal Labor
My due date, April 16th, a Thursday, arrived with our baby boy still nestled safely inside, healthy and content. By 40 weeks, I felt – and certainly looked – incredibly pregnant, my anticipation to meet our little one reaching an almost feverish pitch.
For weeks, I’d experienced Braxton Hicks contractions, but on the night of my due date, they intensified noticeably. Could this finally be it? I messaged the midwives, urged Daniel to an early bedtime, and felt a surge of excitement and nervous energy. The prospect of active labor, a natural birth, and finally meeting our son was exhilarating.
By Friday morning, the contractions were undeniable, coupled with signs of losing my mucus plug. They lasted a minute each, initially spaced about ten minutes apart. I quickly updated my doula and midwives, convinced this was the onset of early labor. I truly believed our baby would arrive that day! Yet, as the day progressed, they spaced out, only to pick up again to ten-minute intervals by Friday night. Perhaps Friday night would usher in real, active labor?
By 3 AM, contractions were a minute long and a mere four minutes apart – typically the “real deal” pattern. But it didn’t last. They frustratingly spaced out again to ten or twelve minutes. Just enough to prevent active labor, but agonizingly disruptive to any chance of sleep. This pattern, the hallmark of prodromal labor, was beginning to take its toll.
Saturday morning brought another resurgence of contractions. Utterly confused and desperate for clarity, I texted the midwife. She kindly invited me to the birthing center for a check. Baby’s head was indeed very low, and I was almost fully effaced, but to my dismay, I was only 2 centimeters dilated. And predictably, the contractions began spreading out once more.
It was unequivocally prodromal labor, often called “false labor.” It mimicked the sensation of true labor, but rather than progressing steadily, it would intensify and then recede, trapping me in an exhausting cycle of anticipation and disappointment. The emotional and physical drain of this prolonged early phase began to weigh heavily.
That evening, after updating my doula, I embarked on a relentless circuit of exercises and stretches, desperate to nudge things along. Bouncing on the birth ball, curb walking, and sipping copious amounts of raspberry leaf tea – all performed as contractions once again picked up their pace. My desire for “the real thing” was overwhelming; I was utterly fed up with days of contractions averaging ten minutes apart. The constant tracking had become a maddening obsession, each inconsistent pattern chipping away at my resolve.
Saturday night delivered another brutal experience. The contractions intensified, making sleep an impossible luxury. By 3 AM, I was groaning in pain, inadvertently disrupting Daniel’s sleep too. They were stronger, closer, but still lacked the crucial consistency needed for active labor.
Sunday morning, the cycle repeated. Back at the birthing center, a different midwife confirmed slight progression in effacement and dilation, but it was minimal, insufficient for the effort expended. I was utterly exhausted and profoundly frustrated. It was then that the midwife unequivocally confirmed it was prodromal labor and gave me crucial advice: I needed to do everything possible to relax and rest before true active labor began. “Eat a nourishing meal, unwind, prioritize sleep, and stop trying to rush your body,” she urged.
Hearing that felt like an immense weight lifting from my shoulders. The permission to go home, to stop obsessively tracking contractions (especially as they were spreading out again), to simply relax and finally get a decent night’s sleep before active labor commenced was a profound relief.
Throughout my pregnancy, I’d often heard how maternal exhaustion during early labor was a primary reason for hospital transfers from natural birth settings. I had resolved early on to prioritize rest during this phase. I knew that failing to do so would significantly increase my risk of a much harder labor. So, I surrendered. I stopped trying to force my body out of prodromal labor and simply allowed it to be. I desperately needed to sleep that Sunday night.
The Irreversible Shift into Active Labor
Sunday evening, I settled onto the couch, engrossed in Top Chef and savoring a warm bowl of soup, when a sharp wince escaped me. The contractions were returning, harder and faster than before, an undeniable shift in their intensity.
Around 7 PM, I attempted to go to bed, willing the contractions away. I needed that sleep so badly. After two nights of broken rest due to relentless contractions, I yearned for at least a few hours of solid sleep. But it was too late. The inevitable had arrived.
I was unmistakably in active labor. Contractions came fiercely and rapidly as Daniel squeezed my hips, a supportive anchor through each wave of pain. It was then that he suggested, “We need to call the doula.” Call the doula? No. I resisted. I still clung to the desperate hope of sleep. Yet, almost instantaneously, our doula was by my side, her calm urgency cutting through my exhaustion: “We need to get in the car, now.” It was a whirlwind of emotions – a surge of excitement mingled with an “oh crap” realization. Here I was, plunging into natural labor at 10 PM, utterly deprived of sleep, facing a night of intense labor, praying for a swift arrival.
The Struggle at the Birthing Center
Upon arriving at the birthing center, the initial check brought disheartening news. I was 100% effaced, baby’s head was at -2 station, but my dilation was a mere 3 centimeters. The midwife gently suggested it might be best to labor at home for a while longer. As another powerful contraction hit, tears welled up. I was in agony, beyond exhausted, and just yearned for swift progression. My plea to stay was granted; I remained at the birthing center.
I found solace and a measure of relief laboring in the warm tub, where I spent the majority of the night. The contractions were hard and fast, and despite being utterly drained, I truly felt I was making significant progress. Around 2-3 AM, a new phase began: I started throwing up, a classic sign that I was transitioning to the most intense stage of labor.
Another check revealed I was still only 5 centimeters dilated. Halfway there, on what was now technically Monday morning, after enduring contractions since Friday. The midwife proposed breaking my water, to which I readily agreed, desperate for any intervention that might speed things up. Post-amniotomy, the contractions escalated in pain, and the sheer exhaustion completely overwhelmed me. The remainder of the early morning hours blurred into a haze of discomfort and fading consciousness.
Around 7 AM Monday morning, as the new midwife began her shift, I somewhat resurfaced into awareness. I remember pleading with her, my voice raw with desperation, asking if she truly believed our baby would arrive today. The thought of enduring another full day of this was unfathomable. This desperate plea for progression became the defining sentiment of my entire labor.
She checked me early that morning, revealing I was 7 centimeters dilated! A wave of relief washed over me. I had progressed from 3 to 7 overnight – only 3 more to go. Exhausted and in pain, yes, but I felt a renewed sense of purpose. I could do this, and she was equally committed to helping me achieve it.
She suggested an IV for fluids and arranged for my chiropractor to come for an adjustment. I labored for a few more hours until my chiropractor arrived, and the adjustment did indeed provide a profound sense of relief, easing some of the pelvic pressure.
Throughout that day, I explored every possible position and method of laboring: in the tub, the shower, on the birth ball, in bed. At one point, in a desperate attempt to accelerate things, I found myself lunging up the stairs, each step a monumental effort. I recall praying and weeping on those stairs, utterly consumed by exhaustion and desperation, trying to physically coax my baby out with his head so low. Lunging up stairs when not pregnant is challenging; doing so 40+ weeks pregnant and in labor is an act of sheer will.
Later, as I labored in bed, they checked me again. To my utter devastation, I had not dilated a single centimeter further the entire day. The uterus, like any other muscle, can become utterly exhausted. My body had simply given up. I watched the light fade from the window, realizing I was heading into yet another night, my baby still struggling to make his entrance, and my water broken for the entirety of the day.
The midwives and my doula were incredible, tirelessly working alongside Daniel and me. We all pushed our limits, but my body had reached its absolute breaking point. A profound fear for my baby consumed me. My poor little one, who must have yearned for peace and quiet, was enduring days of intense labor alongside me. He felt every contraction. How was he coping? Was he as distressed and exhausted as I was? I couldn’t bear to put either of us through another night without tangible progression. All I wanted was for my baby to be safe, healthy, and finally in my arms.
I made the agonizing decision. “I’m done,” I declared. “I cannot continue without an epidural. I cannot endure another night with my water broken.” The raw truth was, neither of us could survive another night of this ordeal.
It was an incredibly difficult choice. The hospital environment was an unknown quantity. What were their COVID-19 policies? Would I have to labor in a mask? Would I be separated from my baby? The uncertainty was terrifying. But a deep, maternal instinct told me that Jett and I needed to go. And so, we did.
The Unexpected Hospital Transfer
By the time we arrived at the hospital, I was beyond mere exhaustion. It was late Monday night, I had been in prodromal labor since Friday morning, and I hadn’t truly slept since Saturday night (and even then, contractions had significantly interrupted my rest). The transition from a serene birthing center to a bustling hospital felt jarring and alien.
I had absolutely no idea what a hospital birth entailed. My preparations had been solely for a natural, unmedicated labor. An epidural, Pitocin, hospital protocols – none of it was part of my plan. Yet, at that moment, I desperately needed that epidural. I needed to relax, to allow my body to progress. The prospect of it was terrifying, but honestly, the immediate cessation of contractions, after enduring them without any pain relief for days, felt like an indescribable miracle.
Then began the process of settling in. Daniel and I were both required to wear masks, a stark reminder of the pandemic’s grip. Jett and I were hooked up to monitors; my blood was drawn, my temperature taken. The results were concerning. My contractions had dramatically spaced out due to extreme fatigue, signaling a lack of progress. My white blood cell count was alarmingly high, I had a fever of 100.4 F, and most frighteningly, Jett’s heart rate was decelerating with contractions. My heart plummeted when I heard his heart rate was struggling. A fever? Were they going to suspect an infection and take my baby away? Fortunately, the medical team concluded it was likely an infection due to my water being broken for such an extended period, which made perfect sense. Both my body and Jett were clearly at their limits.
The OB arrived around midnight, cautiously giving me a 50/50 chance of requiring a C-section. However, he was willing to give me the night, administering Pitocin to try and stimulate contractions for that final push, hoping to turn the corner towards a vaginal delivery. At that point, all I wanted was for us both to be safe and healthy; I was prepared to do whatever was necessary. But I was also committed to trying through the night if the OB believed there was a chance.
My meticulously planned natural birth had morphed into a complex medical landscape: a penicillin IV, an epidural, Pitocin, artificial amniotic fluid for Jett, and internal fetal monitoring. Adding to the ordeal, not long after arriving at the hospital, I started throwing up again.
Throughout the night, nurses constantly rotated my limp body, attempting to stabilize Jett’s vitals, as the epidural rendered me unable to move. They continually adjusted the Pitocin, as Jett continued to struggle with the induced contractions. It was then they discovered meconium in my amniotic fluid, informing me that NICU nurses would need to be present during pushing, in case he inhaled it. Gutted, terrified, and consumed by anxiety, I endured the entire night.
With the profound numbness and sheer exhaustion from the epidural, I had no idea how I would know when it was time to push. But by Tuesday morning, a new sensation began to emerge: increasing pain and pressure. I alerted the nurse, who decided to check me for the first time since our hospital arrival. I offered a silent prayer, hoping desperately for that magical 10-centimeter mark.
She called Daniel over, a joyful lilt in her voice. “Hey, Dad? Are you squeamish? Come see the baby’s hair!” Hair?! She could see his head? She looked at me, a warm smile spreading across her face, and declared, “We’re having this baby, right now!”
The Triumphant Moment: Finally Giving Birth
It was around 7 AM on Tuesday morning, and after days of relentless struggle, it was finally happening. The room rapidly filled with a flurry of medical personnel, their movements a blur. I bombarded them with questions, my voice strained with exhaustion and disbelief: “What’s that?” “Who is that?” “How do I know when to push?” My night nurse, who had been an absolute angel through my horrific night, chose to stay beyond her shift, wanting to see me through to the end. Her compassion was a beacon.
Everything was swiftly prepared. The OB was present, and the nurse calmly instructed me on the pushing technique, despite my limited sensation. I pushed with every ounce of strength I could muster. Less than ten minutes passed when they urged, “Look down, he’s almost here!” Exhausted beyond measure, I simply mumbled, “Nope,” unable to even move my head. With one final, monumental push, they told me to reach down and catch my baby. My baby? I was in shock. There he was – a tiny, screaming bundle of life. My son. The same little being who had inhabited my belly for 40 weeks and 5 days. And despite the harrowing journey, he was healthy, perfect, and utterly beautiful.
They immediately placed him on my chest, and once again, I couldn’t stop talking, a torrent of questions pouring out. I was simultaneously out of it, profoundly exhausted, and utterly thrilled. He was born on April 21st, at 7:38 AM, weighing 7 lbs 4 oz. He was sweet, flawless, and everything I had dreamt of.
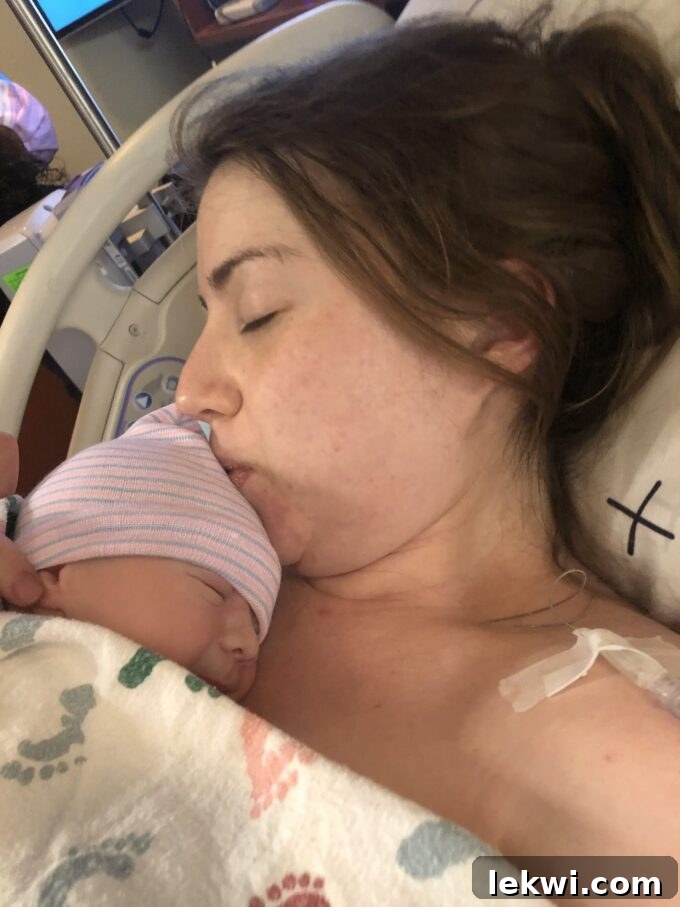
Cradling him, lost in a daze of awe, I vaguely noticed the OB stitching me up. I was too numb and exhausted to ask or even care about the details, but I overheard talk of a second-degree tear. In that moment, the tear and the stitches were utterly insignificant. They could stitch me up however they pleased. All that mattered was that my baby was safe, healthy, and finally in my arms, on the outside.
Navigating Postpartum During a Pandemic
I’m still very much in the thick of it, even now! The immediate aftermath at the hospital proved challenging. We had to remain for two additional nights for monitoring due to the prolonged rupture of my water, necessitating vigilant checks for infection. Nurses would take my blood at 2 AM, while my brand-new baby demanded to nurse through the night, making sleep and recovery from my impossibly long labor a distant dream.
The true work began upon our return home, a home that remained firmly under lockdown. While thoughtful family and friends dropped off nourishing meals, the postpartum experience was nothing like we had envisioned. It was just the three of us, navigating the immense challenges of new parenthood without the hands-on support we had anticipated. The lack of broader familial and social support during this vulnerable period was profoundly difficult.
I had to simultaneously recover from an arduous labor, allow my stitches to heal, learn the intricate dance of nursing, and brave countless sleepless nights with a newborn. Somewhere along the way, I sustained a severe burn to my esophagus during labor – whether from the extensive vomiting or perhaps related to the pain relief and antibiotics for my ruptured membranes, I’m not entirely sure. Even simple sips of water caused searing pain. I ultimately required a prescription to heal my throat before it returned to normal. It was an unexpected and agonizing complication.
Undoubtedly, having a baby during a global lockdown was incredibly hard. Yet, amidst the difficulties, there emerged so many unexpected positives. We were granted an abundance of precious bonding time with our sweet boy. Daily skin-to-skin cuddles became a cherished ritual, my milk supply was robust, and he regained his birth weight and more in record time! The circumstances were unforeseen and challenging, but I will forever treasure those early days – just Jett, mommy, and daddy, forging an unbreakable bond in our own little bubble.
Future Family Plans: Will There Be Another Natural Birth?
Daniel and I are still undecided about having a second baby. We’re committed to navigating this first year of parenthood before seriously considering expanding our family. Should we decide to have another, I honestly have no idea what approach I would take for the birth. It’s a bridge we will cross only if and when we arrive at it.
The Prospect of Recurring Prodromal Labor
Not necessarily. Both my midwives and the OB informed me that prodromal labor could potentially recur in subsequent pregnancies, but they emphasized that every birth is distinct and unpredictable. The unique dance of each labor unfolds in its own way.
Our Unforgettable Journey
And that, in its entirety, is our story. I firmly believe that everything unfolds precisely as it’s meant to, guided by a higher plan. It’s a long, crazy, and undeniably hard story, but it is unequivocally ours. It’s the extraordinary narrative of how my little boy entered the world, and for that profound reason, it remains a truly beautiful tale of resilience, love, and unwavering spirit.
